If you’re looking to improve your diastasis recti (DR), you’re not alone. It’s estimated that up to half of all women experience DR to some degree after giving birth. DR can be difficult to overcome—but mama, don’t lose hope! There are lots of resources to help you heal and fix diastasis recti years later—let’s dive in. It is truly never too late to heal your DR.
Healing Diastasis Recti Years Later: 8 Top Tips
From understanding and assessing your diastasis recti to engaging the right muscles and the right support system, the following strategies will help you find the results you’re seeking.
1. Understand the Issue
Let’s start by answering a few common questions.
What is diastasis recti anyway?
Diastasis recti is a thinning of the connective tissue, the linea alba, that runs between your rectus abdominis, or “six-pack” muscles. It often occurs during pregnancy, and truth be told, it’s the body’s brilliant way of making room for a baby.
All pregnant women experience DR–it’s a normal and necessary process. Sometimes it spontaneously heals in early postpartum, but for many women (me included!), it takes time and effort. And for nearly 1 in every 2 women, the condition results in some degree of ab separation or gap after the six month postpartum time frame.
Does diastasis recti (ever) heal itself?
You might be wondering: does diastasis recti ever go away? Well, it depends. For some women, the condition does heal on its own in a relatively short period, especially during the first six months postpartum. But for many women, improving DR can require targeted fitness and awareness-building. In both cases, directly addressing the condition of abdominal separation, with a focus on your deep core muscles, can speed up and improve recovery.
What happens if you don’t heal diastasis recti?
While having DR doesn’t necessarily mean that you’ll have other postpartum concerns, it does indicate a pressure imbalance within the body. Unaddressed, many women also experience a number of pressure-system conditions including a weak core, umbilical hernia, incontinence, discomfort during sex, and pain in the back, pelvis, and hips.
Can you heal diastasis recti years later? Really?
Yes, ma’am. Intervention programs including transverse abdominis activation with an exercise program, coordinated breathing exercises, and pelvic floor muscle engagement can yield positive outcomes. You could also ask these women about their personal experiences—each improved their DR using SLAM.
2. Assess Your Diastasis Recti
Whether or not your doctor checked you, you’ll want to do a diastasis recti self-check.
During self-assessment, be sure to lift your head and shoulders off the ground as little as possible. If you sit up too far, results could indicate that your rectus abdominis muscles, or “outer” abdominal wall, are closer together than they really are. You’ll need to check for width and depth—understanding the tension on that tissue matters.
3. Take Some Deep Breaths
Don’t freak out if you do have an “unclosed diastasis recti.” The truth is, we all have some level of separation even before babies. If yours is 2+ fingers deep or lacks tension, we can improve it!
You can fix diastasis recti even after time has passed. And one of the most important tactics to healing your foundational core, loving your mommy tummy, and repairing a persistent belly pooch is breathwork.
It comes down to managing intra-abdominal pressure. Basically, your core is a pressure system. Your diaphragm sits under your rib cage, and ideally, as you inhale, this dome-like muscle flattens against your abdominal organs and pushes air down into your lungs. This gentle expansion also lets the pelvic floor muscles relax. When you exhale, the diaphragm recoils and the pelvic floor gently lifts.
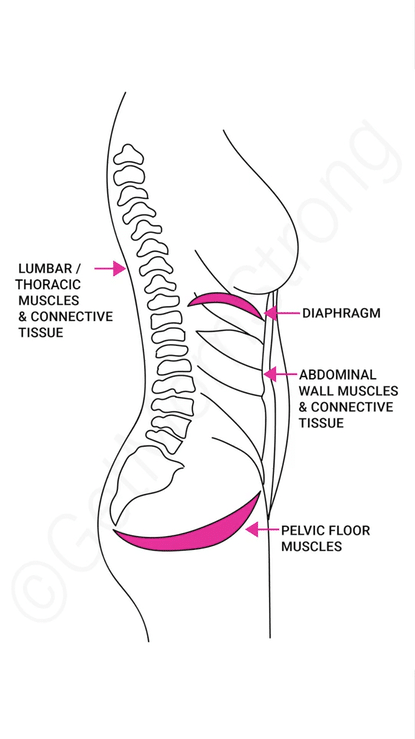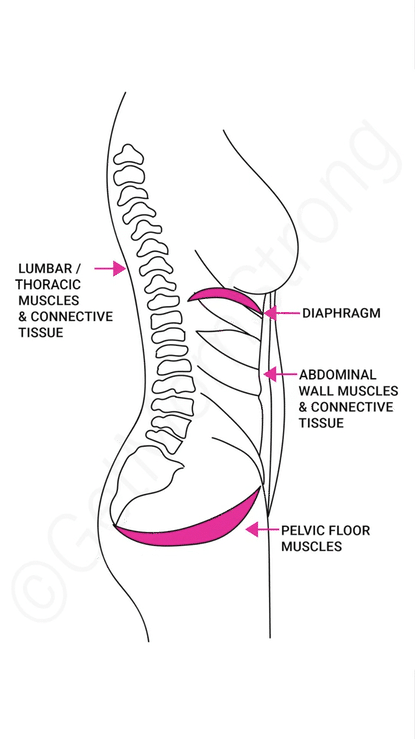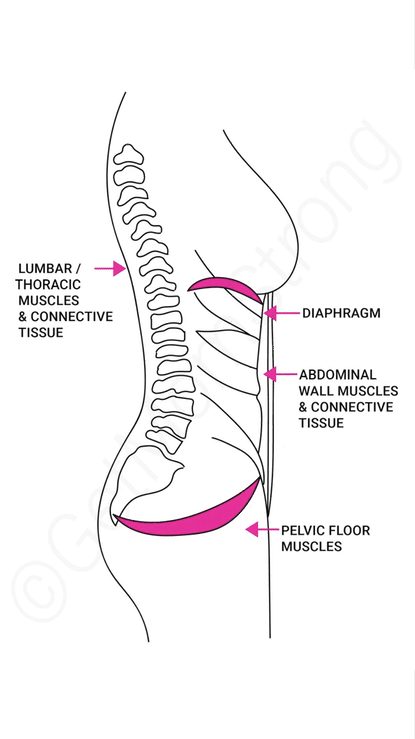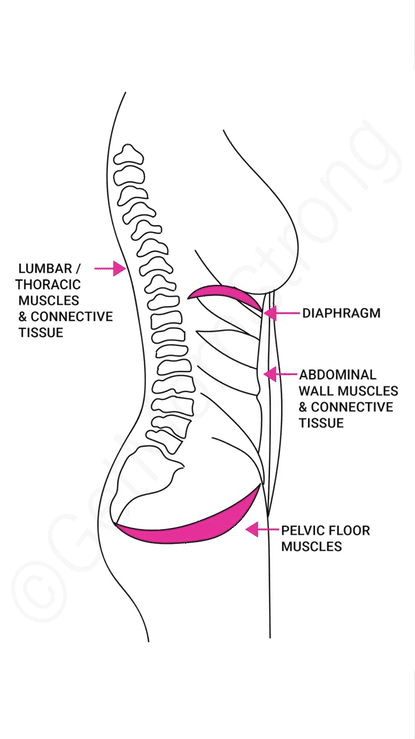
Unfortunately, many of us suck in our tummies and grip our ab muscles, which can make us breathe backwards—essentially, we start to breathe up into our chests. The video below details how to get back to breathing right:
This is especially important when you exercise, to avoid bearing down on the pelvic floor.
4. Increase Your Rib Mobility
Improving DR is all about breathing down into your body—and increasing your rib mobility will help you do this better.
A few approaches to increasing rib mobility include manually expanding the rib cage, mobilizing the latissimus dorsi muscles (or lats), and opening up the back muscles. You’ll find corresponding exercises, including skin rolling, foam rolling, back expansion, and wall mobility slides, in the video below. Also, getting a massage can really help—treat yourself!
5. Strengthen Your Deep Abdominal Muscles
One important strategy for healing DR is strengthening the deepest layer of your abdominal muscles, the transverse abdominals. These core muscles sit beneath your six-pack muscles and wrap all the way around your torso, from top to bottom.
If you can get this supportive abdominal system to help keep things in their place, your connective tissue is going to be much more likely to heal. Plus, increasing strength in your transverse abdominal muscles with core exercises will help reduce back and pelvic girdle pain, and improve your posture. I designed the Core Basics program around exercises that target this muscle group (through deep core work) for optimal results.
6. Practice Mindfulness
Improving awareness of how you breathe and hold your body can make a big difference. Healing DR is not about keeping your core engaged all the time—it’s about learning to activate and keep your core stable for mom-life tasks. Over-activating your abdominal muscles can actually cause more harm than good, especially for women with pelvic floor issues.
Focus on your natural body alignment. Think of your body like a snowman—with head, ribs and pelvis all stacked. Whenever possible in your daily life, square your hips and aim for a neutral spine.
What we do in the 23 hours outside our exercise routine makes a huge impact on postpartum healing. Especially when it comes to daily tasks like picking up kids (and picking up all their stuff) with good posture. The two most common postural compensations when lifting heavy things are to jut out a hip or sway back, arching your low back and tightening your butt. Here are a few tips to help you maintain proper posture and awareness, no matter what madness is happening.
7. Give Yourself Time
Healing takes time so remember to be patient with yourself. Every woman’s body is different. A focus on losing weight or rushing to get back to a pre-baby body, especially by overdoing exercises like crunches and sit-ups, can actually make DR separation worse. And, please know that no matter how far out postpartum you are (yes, postpartum is forever, even if your kids are 35), it is never too late to heal and improve DR.
8. Seek Out Extra Support
If you’re able to, go see a pelvic floor physical therapist. Physical therapy can make a big difference in many areas of women’s health.
Also, check out the SLAM Program. There’s really nothing else like it for postpartum empowerment and healing, especially if you’re looking to improve diastasis recti. I’ve been there and I know how hard it can be – I also know the answer doesn’t include crazy exercise regimens or extreme weight loss and dieting. Let’s get you feeling and looking great…together, the right way. Learn more.
